- 46 yr old male patient was brought to the Emergency Department with a sudden episode of loss of consciousness. Attenders gave the history of generalized tonic–clonic movements, associated with up-rolling of the eyes, tongue bite, and urinary incontinence. This was followed by unresponsiveness after which the attenders rushed to emergency.
- There is a history of multiple similar episodes in the past and the patient was not taking any treatment for the same.
- There was fracture in the left wrist along with dislocation of thumb.
Intracranial dermoid cyst
- fat-containing, usually midline.
- May rupture, causing fat droplets in subarachnoid space.
- On MRI: fat signal similar to lipoma, but often lobulated with mixed intensity due to hair, keratin, and calcifications
Teratoma (mature)
- Contains fat, calcification, and sometimes teeth/bone.
- More heterogeneous than lipoma on MRI.
- Often associated with mass effect.
Fat-containing glioma or other neoplasm
- Certain tumors (e.g., oligodendroglioma, ependymoma) may rarely contain fat or lipidized cells.
- Usually not as homogeneous as lipoma and often enhance with contrast.
Calcified midline tumors or malformations
- Oligodendroglioma, pineal region tumors, or meningioma can have calcifications and mimic lipoma in non-fat-suppressed images.
- CT helps differentiate fat from calcification.
Lipomatous hypertrophy of the corpus callosum
- Fat deposition within the corpus callosum itself, though extremely rare.
- MRI shows diffuse, infiltrative high T1 signal without a discrete capsule.
A rare, congenital, benign lesion composed of mature adipose tissue located within the pericallosal cistern, closely related to the corpus callosum. It is a developmental anomaly rather than a true neoplasm.
Epidemiology
- Represents <0.1–0.5% of all intracranial tumors.
- Common location: Along the corpus callosum, particularly pericallosal region.
- No significant sex predilection.
- Often detected incidentally during imaging for seizures, headache, or other neurological complaints
Etiopathogenesis
- Originates from abnormal differentiation of the primitive meninx (mesenchymal derivative of neural crest cells) during embryogenesis.
- Normally, the primitive meninx should resorb and be replaced by subarachnoid space. Failure of resorption results in persistence and differentiation into adipose tissue.
- Frequently associated with corpus callosum anomalies (agenesis, hypogenesis, or dysgenesis), which develop from the same embryonic midline structures.
Clinical Features
- Many patients are asymptomatic.
- When symptomatic:
- Seizures (most common presenting complaint, often generalized tonic–clonic)
- Headache
- Cognitive impairment or developmental delay (especially in children with associated callosal agenesis)
- Rare: focal neurological deficits, behavioral changes
- Symptoms usually result from associated malformations rather than the lipoma itself.
Imaging Findings-
- CT
- Well-defined, homogeneous, hypodense lesion (-50 to -100 HU, consistent with fat).
- May show peripheral or central calcifications (~50% cases).
- No enhancement with contrast.
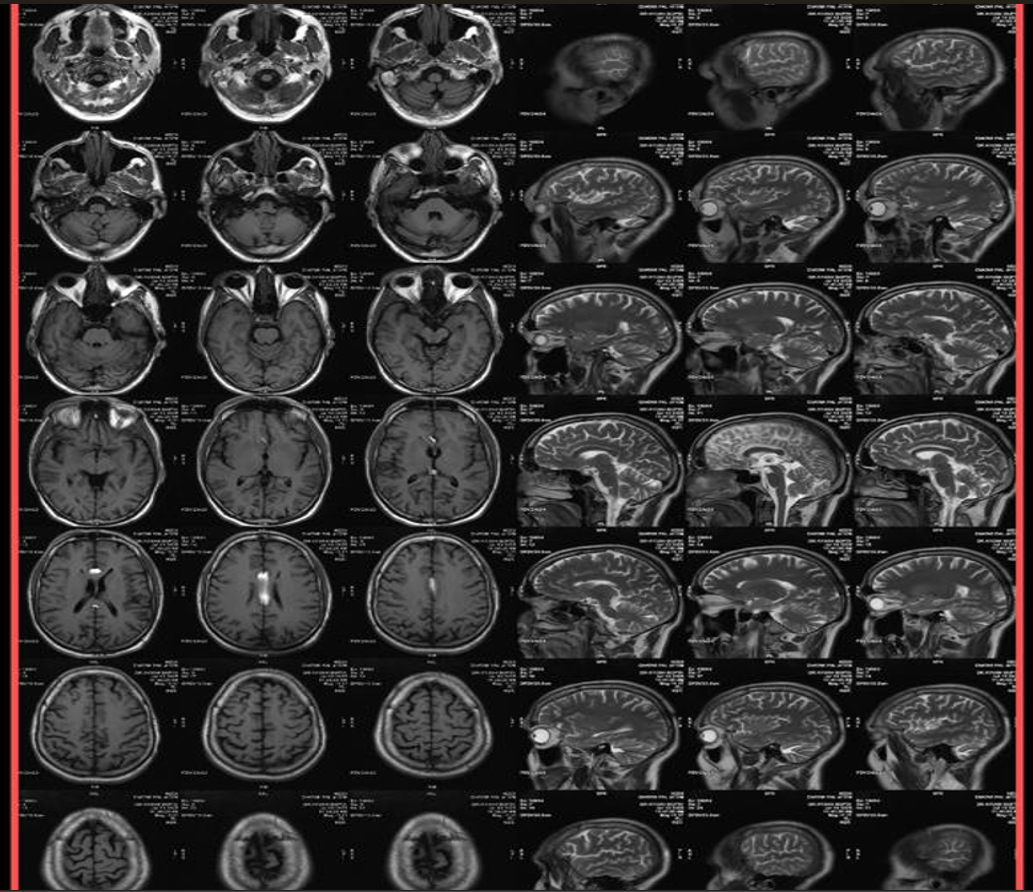
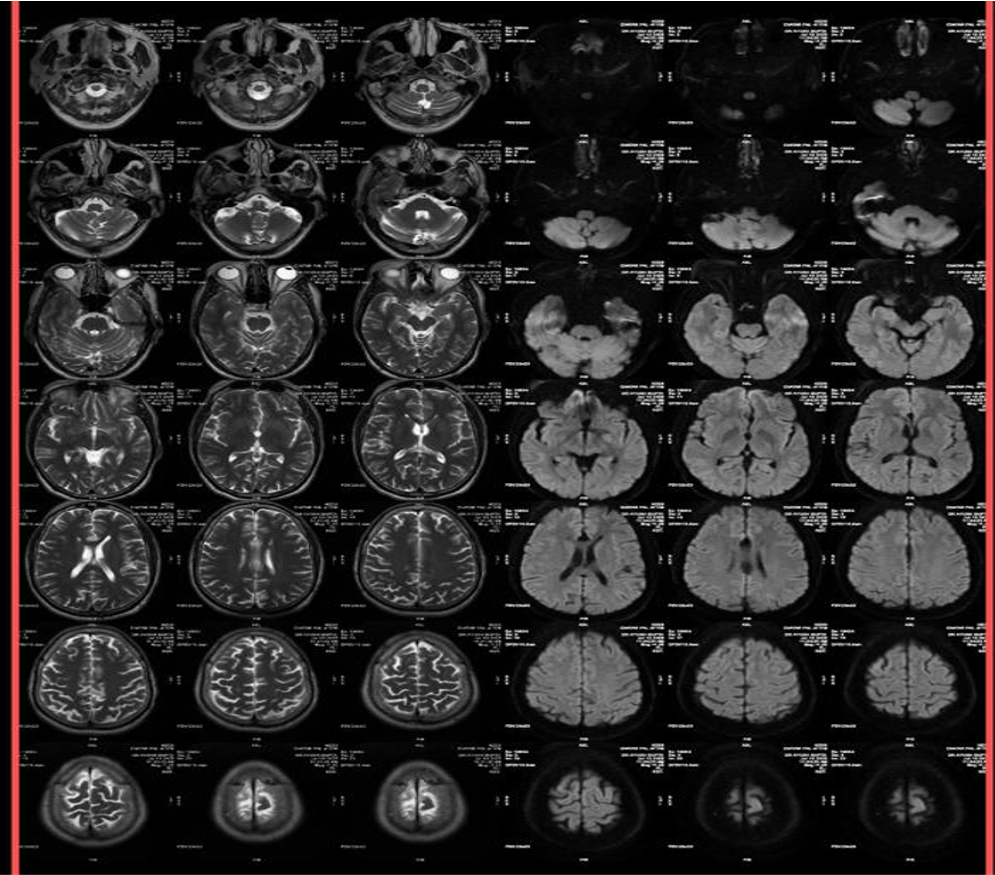
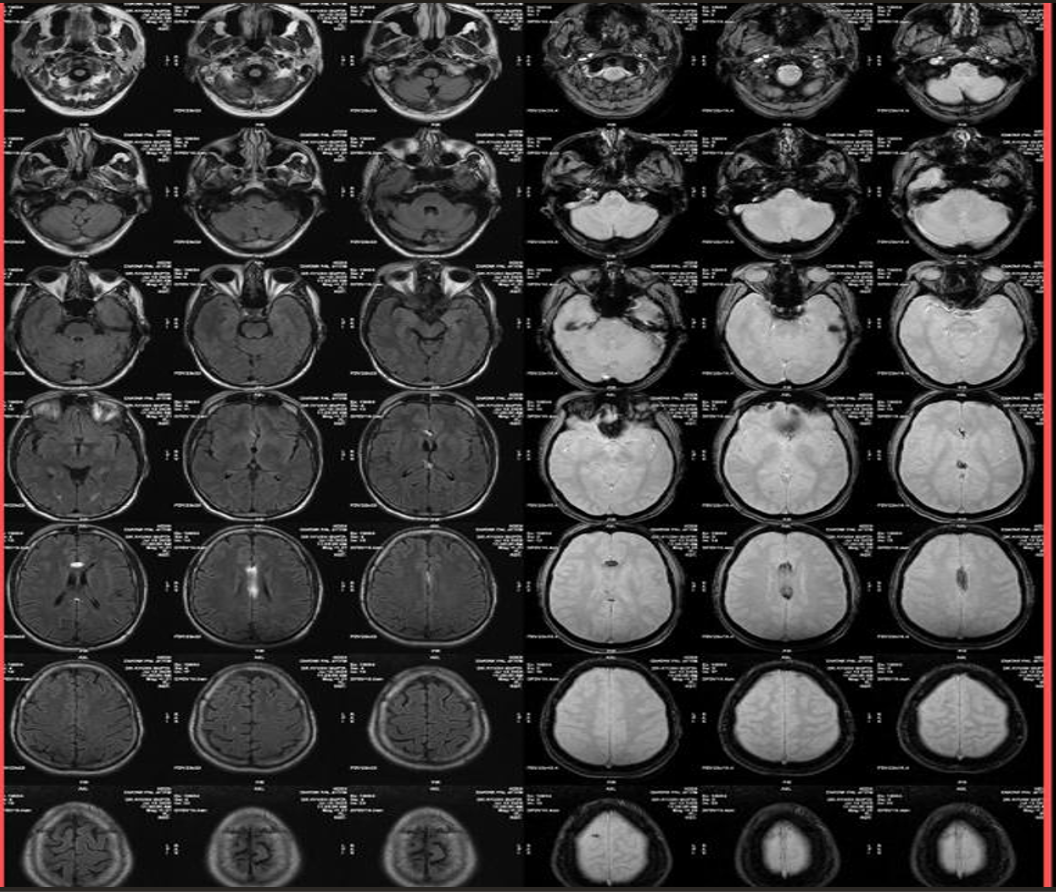
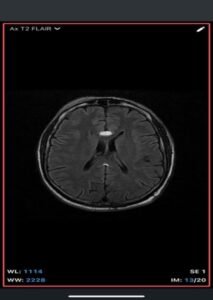
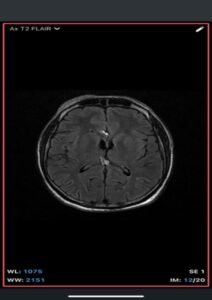
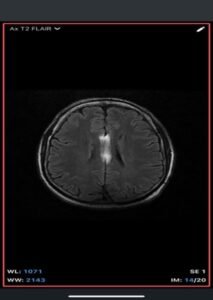
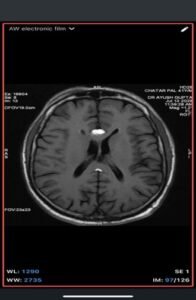
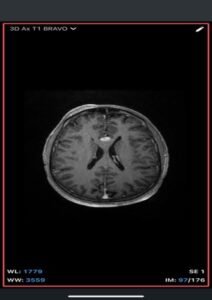
- MRI
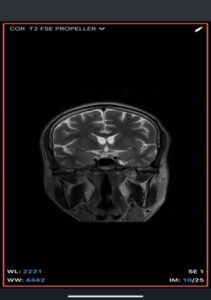
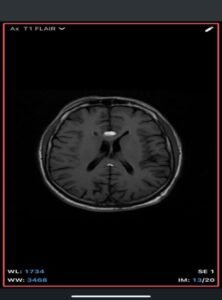
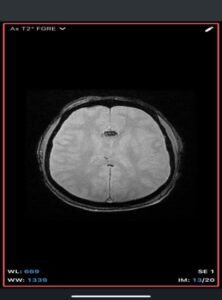
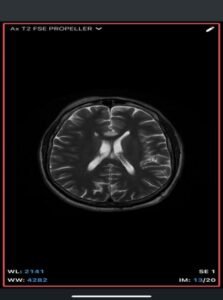
- T1-weighted: Hyperintense (fat signal).
- T2-weighted: Variable, usually hyperintense; may show chemical shift artifacts.
- Fat-suppressed sequences: Complete signal suppression confirms fat composition.
- Post-contrast: No enhancement.
- Often associated with:
- Corpus callosum agenesis/dysgenesis
- Interhemispheric cysts
- Calcifications (better on CT)
Management
- Asymptomatic cases:
- No surgical intervention (lesions are highly vascular and adherent to surrounding neurovascular structures → high risk).
- Symptomatic cases:
- Symptom-directed therapy (antiepileptic drugs for seizures).
Neurosurgical intervention only if secondary complications (very rare).